- Austausch & Vernetzung
- Wissen & Lernen
- Advocacy
- Unsere Themen
Aktuelle Kurznachrichten zu Themen der internationalen Gesundheitszusammenarbeit sowie zu Informationen unserer Mitglieder.

"Im zentralafrikanischen Tschad ist die Müttersterblichkeitsrate rund 140-mal höher als in der Schweiz. Die Berner Organisation Women’s Hope International hat eine Hebamme portraitiert, die sich mit einfachen Mitteln aber viel Herzblut für sichere Geburten in ihrer Heimat einsetzt."

Conflict, climate disasters and regressive reproductive rights deny pregnant women access to a doctor or midwife, Save the Children reports
"Women in countries affected by conflict are three times more likely to go without a skilled birth attendant, and three times more likely to give birth outside of a health facility, according to a new report by Save the Children. Climate disasters and regressive reproductive rights and education are also denying pregnant women access to a doctor or midwife, the charity said."
![IHR Goes into Extra Time: Countries Make Definite Progress on the Amendments to the International Health Regulations, But Not Enough to Close a Deal [WG-IHR8]](/de/assets/image-cache/uploads/images/news/2024/shray-chawla-Qqs8ppyxANw-unsplash.0a13a20e.jpg)
In this story we look at key, contentious provisions on equitable access of medical products and on financing – on which hinges the final deal on the IHR amendments.
"Negotiations on the International Health Regulations go down to the wire as countries were unable to complete the discussions at the end of the final meeting of the Working Group to amend the IHR, that concluded this week. Riding on a constructive approach and an overall positive momentum, countries made steady progress under the decisive leadership of co-chairs Abdullah Asiri and Ashley Bloomfield, but a few areas of contention remained as the clock ticked away towards the conclusion of the meeting on April 26, Friday. The working group decided to buy additional time to conclude the negotiations and are expected to meet on May 16-17 to complete the process. More time is needed to reach consensus on key contentious matters including on technology transfer, a dedicated fund, governance of an implementation committee, among other areas, diplomatic sources said."

Malaria remains a huge health challenge in the African region, which is home to 11 countries that carry approximately 70% of the global burden of malaria.
"In a significant step forward for malaria prevention in Africa, three countries—Benin, Liberia and Sierra Leone—today launched a large-scale rollout of the life-saving malaria vaccine targeting millions of children across the three West African nations. The vaccine rollout, announced on World Malaria Day, seeks to further scale up vaccine deployment in the African region. Today’s launch brings to eight the number of countries on the continent to offer the malaria vaccine as part of the childhood immunization programmes, extending access to more comprehensive malaria prevention."
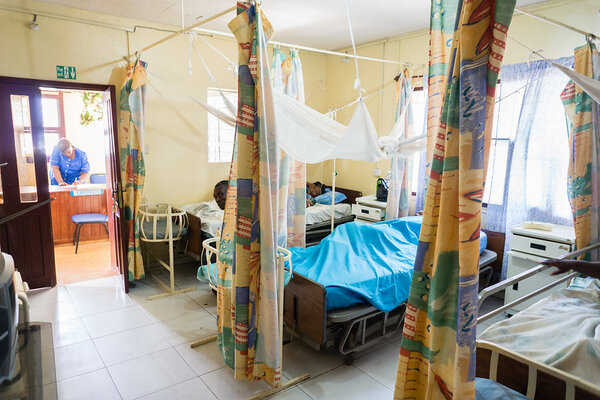
"Mirriam Banda is a midwife, nurse, administrator, counselor and health advocate for 15,000 residents of her community in eastern Zambia at the Kafumbwe Rural Health Center in Katete District. She is married and a mother of three children. In 2011, a severe malaria outbreak nearly cost her daughter her life. The ordeal continues to deeply affect Mirriam, who also battled malaria numerous times during her childhood – so many that she cannot remember the exact number. Today she faces the disease day after day in her work and her community and, in the context of World Malaria Day (April 25), we spoke to her."
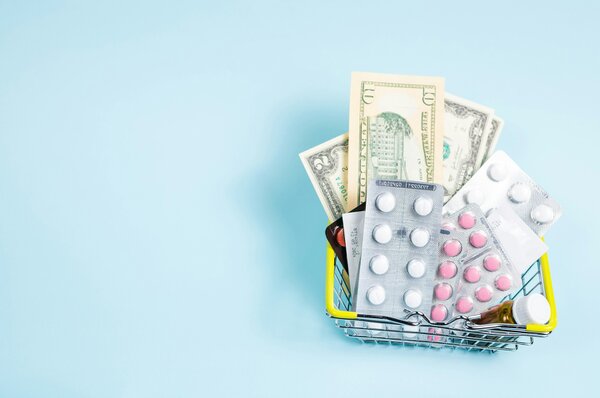
Many lower-income countries are spending less on health than they did before the COVID-19 pandemic at a time when donor funding is on the decline.
"In Washington, D.C., where health and finance ministers, global health leaders, and international funders gathered for the World Bank’s Spring Meetings, these are ways of talking — or not talking — about a growing fear: A large group of countries are facing an alarming health funding landscape. “We have a problem globally,” health economist David Evans said Thursday at a forum on health financing. The problem, Evans said, is particularly acute in a group of 28 low- and middle-income countries whose governments are spending less on health than they did before the COVID-19 pandemic, with no prospect — according to International Monetary Fund projections — of returning to those pre-pandemic levels in the next five years."

"The Board of the Global Fund to Fight AIDS, Tuberculosis and Malaria (the Global Fund) held its 51st meeting this week in Geneva, Switzerland. While anticipating record disbursements this year, with an unprecedented pace of investment in resilient and sustainable systems for health (RSSH) and pandemic preparedness and response (PPR), the Board repeatedly acknowledged the numerous challenges – including climate change, conflict, displacement, geopolitics, the economic situation, and in particular, the erosion of human rights and gender equality – that undermine the Global Fund partnership’s ability to end the three diseases by 2030."

Ein Gastkommentar von Ilona Kickbusch
"Im Zusammenhang mit den Diskussionen der Weltgesundheitsorganisation (WHO) um ein Pandemieabkommen reden Kritiker von einer «WHO-Diktatur». Davon kann keine Rede sein, die Mitgliedländer sind denn auch weit davon entfernt, eine Einigung zu erzielen. Die Fehlinformationen zu den derzeitigen Verhandlungen am Sitz der Weltgesundheitsorganisation (WHO) in Genf nehmen zu. Besonders laut sind jene Stimmen, die einen drohenden Souveränitätsverlust der Nationalstaaten und eine «WHO-Diktatur» am nahen Horizont herbeireden. Sie wissen offenbar wenig über den Standardablauf internationaler Verhandlungen – oder wollen das gar nicht wissen."

"The latest draft of the pandemic agreement, while deferring many operational issues, keeps equity hopes alive in many aspects – including by cementing in-principle agreements on a pathogen access and benefit-sharing (PABS) system, a global supply chain and logistics network and geographically diverse “capacities and institutions” for research and development. The streamlined 23-page draft was sent to World Health Organization (WHO) member states on Tuesday night ahead of the final meeting of the intergovernmental negotiations body (INB) on 29 April."

As the 6th Planetary Health Annual Meeting begins in Kuala Lumpur, Sophie Gepp and colleagues commend progress in the field of planetary health but call for greater accountability of organisations to ensure planetary health justice
"This year marks the 15th anniversary of the first publication of the framework of “planetary boundaries,” which describes the biophysical limits of Earth systems that, if breached, could have devastating consequences for humanity. Six years after this publication, the report of the Rockefeller-Lancet Commission on Planetary Health defined the concept as “the health of human civilisations and the natural systems on which they depend.” Though progress has been made in the field of planetary health, we need stronger commitment and action for justice and transformative change."

"Artificial Intelligence (AI) can save lives – but “we need to get the regulations right,” according to Dr Ricardo Baptista Leite, CEO of HealthAI, the agency responsible for artificial intelligence in health. To address the urgent need for the robust regulation of AI in the healthcare sector, HealthAI has initiated a worldwide community of practice (CoP), the organisation said last week. This initiative aims to strengthen each nation’s capacity to create well-informed regulations that promote AI’s ethical and fair utilisation in healthcare."

New amendments to patent rules in India will jeopardize the country’s ability to produce generics, dealing a strong blow to access to medicines in both India and other countries of the Global South
"India notified amendments to its patent rules on March 15 this year. Despite opposition by patient groups, activists, civil society and academics, the government has brought in changes that will significantly impact India’s ability to produce generic drugs and maintain access to affordable medicines. This will impact not only India, but also other countries which obtain cheaper medicines from India. It is no coincidence that just five days before the amendments were announced, India signed a Free Trade Agreement (FTA) with the European Free Trade Association (EFTA) that comprises Norway, Iceland, Liechtenstein and Switzerland. Switzerland is home to big pharma companies like Novartis, Roche and Bayer and successfully pressured India to accept TRIPS plus measures in the agreement."

Public Consultation Period 7th - 30th April
"Transform Health and partners are convening a period of public consultation on a draft Model Law on Health Data Governance, which articulates core elements, guidance and model legal text, informed by equity and rights-based principles, among other international, regional and national commitments and best practice. The purpose of this consultation period is to gather stakeholder and expert feedback on the draft, including its content and how it is structured. Through this process, we aim to strengthen and validate the draft, while building consensus, alignment and broad support around the core elements."

Africa needs a paradigm shift in healthcare financing in the face of limited resources. Opinion by Dr. Githinji Gitahi, head of Amref Health Africa
"Thirteen years ago this month, member states of the African Union met in the Nigerian capital. They adopted binding commitments to spend at least 15 per cent of their national budgets on health and urged donor countries to increase financial support for the continent’s health sector. What is now known as the Abuja Declaration recognized that Africa’s future rests on the health of its people. In this guest column Dr. Githinji Gitahi, head of one of Africa’s leading health organizations, looks back at that goal and forward at what needs to be done. The Abuja Declaration gives a clear and measurable target, leaving little room for debate. It provides a straightforward metric to assess which countries have met the 15 percent goal, those that haven’t, and those worthy of celebration for their achievements. However, while the spending benchmark is a tangible indicator of a government’s commitment to healthcare, it falls short in addressing the broader determinants of population health."

In Wakiso einem Distrikt in Uganda herrschte eine grosse Impfzögerlichkeit während der COVID-19 Pandemie. Trotz Bemühungen des Gesundheitsministeriums gab es keine Fortschritte. Im Oktober 2022 wurde jedoch ein neues Kapitel aufgeschlagen, als sich eine beeindruckende Allianz zusammenfand. Die Makerere University School of Public Health, die Rockefeller Foundation und Amref Health Africa schlossen sich mit dem Gesundheitsministerium und der Kommunalverwaltung des Bezirks Wakiso zusammen. Ihr Auftrag war klar: Die Village Health Teams (VHTs) sollten geschult und gestärkt werden. Das Ergebnis war beeindruckend und ein Beispiel für die Solidarität der Gemeinschaft: 1.000 geschulte VHTs konnten durch unermüdlichen Einsatz der durch Fehlinformationen geschürten Impfmüdigkeit begegnen und das Vertrauen der Bevölkerung gewinnen. Eine Welle der Veränderung wurde ausgelöst.